Filipino coronavirus patients endure more pain amid drug dearth
By Jenina P. Ibañez and Beatrice M. Laforga, Reporters
IT TOOK Nikko Lae D. Abdon, 30, nearly a week to find medicines for her 66-year-old uncle, who got admitted in an intensive care unit room at the San Lazaro Hospital in the Philippine capital.
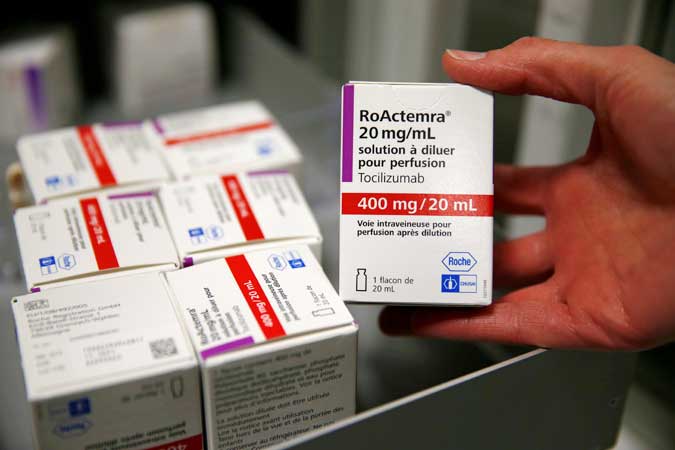
The drug tocilizumab, which is mainly used to treat arthritis, worked wonders to alleviate his pain after he was diagnosed with a severe coronavirus disease 2019 (COVID-19). Doctors also gave him remdesivir, an anti-viral drug originally made to treat hepatitis C.
“We were grateful that the doctors were able to save him,” Ms. Abdon, who works as a nurse at the hospital, said in mixed English and Filipino by telephone. “I didn’t like how we really struggled to find the medicines.”
 “I can only imagine how hard it might be for others to see their relatives suffer because they can’t afford the medicines,” she added.
“I can only imagine how hard it might be for others to see their relatives suffer because they can’t afford the medicines,” she added.
Ms. Abdon said they spent P20,000 for a vial of tocilizumab and P52,000 for six vials of remdesivir at senior citizen discount rates.
Many coronavirus patients in the Philippines have had to pay for expensive medicines to ease their pain as drugs in public hospitals are depleted and given insufficient healthcare insurance coverage from the state.
San Lazaro Hospital — a 500-bed capacity state hospital for infectious diseases — receives only 50-100 vials of remdesivir a week.
These are just enough to treat 16 patients at most, compared with as many as 150 coronavirus patients that the hospital was treating last month, said Rontgene M. Solante, head of the hospital’s Adult Infectious Diseases and Tropical Medicine Department.
“More than 80% will buy remdesivir outside,” he said by telephone. “They have to spend out of pocket since we can’t just let them be without the medicines.”
Local drug companies are trying to order more COVID-19 drugs, which easily run out because of high demand, Beaver Tamesis, president of the Pharmaceutical and Healthcare Association of the Philippines, said by telephone.
“Patients die before the drug becomes available,” he said in mixed English and Filipino. “Supply is slightly behind the demand.”
Demand was particularly high in the past months amid a fresh surge in coronavirus infections — a daily peak of 15,310 on April 2 — that threatened to put the country’s health system on the brink of collapse.
COVID-19 infections in the Philippines were now decreasing, with 6,400 new infections reported on average each day, according to Reuters’ COVID-19 tracker. That’s 59% of the peak — the highest daily average reported on April 15.
About 1.12 million people have been infected with the coronavirus since the pandemic started last year, with almost 19,000 deaths.
INDIAN BAN
Biocare Lifesciences, Inc. a local drug supplier, was caught off guard after India banned remdesivir exports last month after a record spike in cases there. Seven Indian companies have licensed the drug from US-based Gilead Sciences to produce 3.9 million units each month.
The company halted orders from India and continues to import the drug from Egypt and Bangladesh, while other local distributors that mainly import from India could no longer do so.
“We were surprised,” Ronald C. Palacio, Biocare Business Unit head, said in Filipino, referring to the Indian export ban.
He noted that while Biocare could meet the demand from about 250 hospitals, the company started getting more orders from state hospitals that were also affected by the ban. Some hospitals have been trying to stock for their yearly requirements, he said.
“We don’t have a problem with the stocks of remdesivir because shipments were continuously arriving,” he said. But they were caught off guard by sudden orders from government hospitals, which were not part of their plan, he added.
Hospitals can only order remdesivir through a compassionate special permit, while the Food and Drug Administration (FDA) considers it an “investigational” drug. Instead of ordering in bulk based on market demand forecasts, the distributor through each permit can only import the specific quantity ordered by hospitals.
Mr. Palacio said some hospitals had also failed to anticipate the recent surge in cases, which meant that they did not order as much before the Indian ban.
“The hospitals ran out of permits,” he said, noting that orders are limited by the quantities stated in their FDA permits.
Drug makers from other countries have also limited their exports to ensure enough supply in their home countries that have had to deal with the infection spike.
Biocare started importing tocilizumab last month, but its first two shipments have not been enough to meet local demand. The company would try to equally allot supply for a number of hospitals, he said.
The government should consider allowing the emergency use of the drugs so local suppliers could import more, Mr. Palacio said. But products should be screened to ensure quality and consumer safety, he added.
Mr. Tamesis from the pharmaceutical group said supply chain professionals should be able to forecast demand better, perhaps using infection projections.
The supply problem extends to medications for anxiety disorders, he said.
“It’s a very common feedback from those under my care,” Joan Mae Perez-Rifareal, a psychiatrist who works in Quezon City, said in mixed English and Filipino.
“They say ‘Doc, we looked through every drugstore near our residence and it has run out,’” she said by telephone, noting that patients looking for psychiatric services have increased during the pandemic.
Ms. Rifareal said some people are stressed about their transition to work from home or distance learning, while others are just anxious about the uncertainties from the health crisis.
There’s also been a dearth in high-tech machines needed by patients with severe coronavirus to boost their oxygen levels and help them survive, San Lazaro Hospital’s Mr. Solante said.
The hospital only has 30 high-flow nasal cannula devices and 20 ventilators, compared with as many as 100 patients needing them. Patients who are forced to rely on regular nasal machines are more likely to die.
“We use the high-flow nasal devices on a first come, first served basis because it is unethical if we choose who will get the machines and those who don’t,” Mr. Solante said.
The problem can be traced back to the country’s reliance on imports, making the machines difficult to get and expensive for both public and private hospitals to stock up on.
The prices of these devices have gone up by 67% to P500,000 each from last year because of high demand and tight supply, Mr. Solante said.
Ms. Abdon is thankful that her uncle survived without the machine. As a nurse, she’s worried about other patients who may not be as fortunate.
“This May, we’re hoping the daily cases will continue to go down,” she said. “Nurses, doctors and other medical staff here are getting exhausted.”



