Traditions compete with science for vaccine hesitancy among indigenous people in PHL
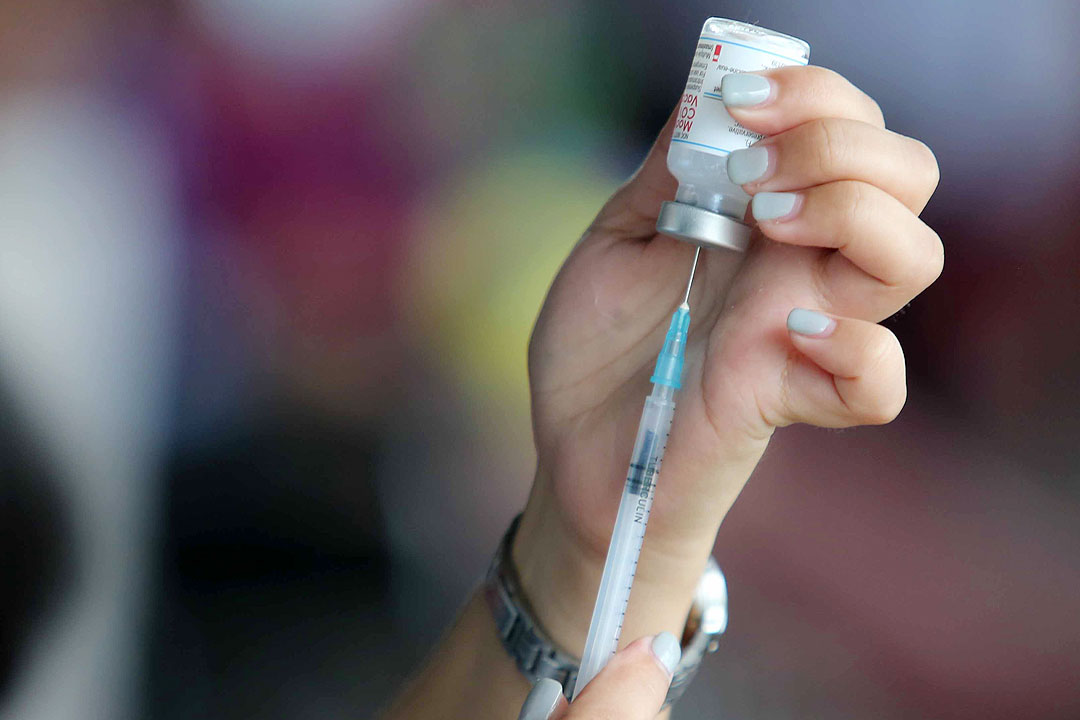
By Luisa Maria Jacinta C. Jocson
MARCELINO S. TENA, a tribe leader of the Dumagat community in Quezon province south of Manila, the Philippine capital, is wary of vaccines.
“Indigenous people (IP) are scared of injections,” he said in a Facebook Messenger chat in Filipino. “Since the coronavirus lockdown began, we IPs have been afraid of getting sick, infecting others and potentially dying of the virus.”
Members of the sea-faring indigenous group do wear face masks and keep their distance as a health protocol, but only when they leave their homes to go to the city.
 “We don’t wear face masks in our community so we can continue to breathe the fresh air, fish in our waters and eat healthy food,” Mr. Tena said. “This is how we stay strong.”
“We don’t wear face masks in our community so we can continue to breathe the fresh air, fish in our waters and eat healthy food,” Mr. Tena said. “This is how we stay strong.”
More than 67 million of about 110 million Filipinos have been fully vaccinated against the coronavirus disease 2019 (COVID-19), about 13 million of whom were also injected with booster shots, according to the Health department.
In contrast, only 1.07 million of about 22 million indigenous people have been fully vaccinated, which is a concern as a fresh surge in infections are again sparking lockdowns in several countries including China, where the coronavirus is believed to have originated.
The government is racing to vaccinate more people as it reopens the economy and protect its population from future coronavirus variants.
The Philippines might experience another surge in coronavirus infections by May or June, similar to what other countries are experiencing now, according to the OCTA Research Group from the University of the Philippines.
Most indigenous communities follow health protocols, though they mostly stay in their areas, said Roda Tajon, a program coordinator at the Philippine Task Force for Indigenous Peoples’ Rights (TFIP).
“IPs feel safer in their communities,” she said in an e-mail. “They seldom go out and get exposed to infections.”
While indigenous peoples’ traditional lifestyles are a source of their resiliency, these can also pose a threat during a pandemic, according to the United Nations. “For example, most indigenous communities regularly organize large traditional gatherings to mark special events e.g. harvests, coming-of-age ceremonies, etc. Some indigenous communities also live in multi-generational housing, which puts indigenous peoples and their families, especially the elders, at risk,” it added.
In many areas in the countryside, indigenous tribes treat illnesses with herbal medicines found in their ancestral lands.
“These are found to be very effective and safe,” Ms. Tajon said. “Aside from using herbal medicines, they are seldom exposed to COVID-19 cases because they usually spend their days on the farm. It was only when outsiders and returning residents came that cases escalated.”
While the capital region experienced a slew of back-and-forth lockdowns, IP communities were, for the most part, untouched by the pandemic frenzy.
“Within our ancestral domain, especially in the inner barangays, the pandemic did not affect their lives that much,” Maria Angelica P. Umingli, an Isnag from Kabugao, Apayao, said in a text message.
When a surge did occur within the Isnag community, rural health and disaster agencies moved quickly to contain the outbreak.
Ms. Tajon said pandemic lockdowns had affected indigenous people’s livelihood and worsened their lack of access to social services such as healthcare given their remote locations.
“Without any health workers present, IPs opted for self-treatments to common illnesses,” she added.
Vaccine hesitancy in these communities is common, largely due to the lack of health education.
“IPs are hesitant in receiving vaccines because they’re afraid of the supposed side effects. The Dengvaxia scare and disinformation on social media are also not helping.”
In Palawan and Mindoro provinces, indigenous people are afraid to visit rural health units for common ailments such as cough and colds for fear that they could get diagnosed with COVID-19, Ms. Tajon said. Some in Luzon and the Visayas avoided seeking treatment because they might be required to undergo testing that they can’t afford.
“The lack of state healthcare workers for IPs also forced them to seek private doctors, which often left them indebted,” Ms. Tajon said.
In a study by the TFIP, pregnant indigenous women bore the brunt of the COVID-19 pandemic.
“Even before the pandemic, the ban on home birthing made it difficult for indigenous women to allocate resources and prepare,” according to the report.
Travel restrictions and testing requirements became more burdensome forcing them to leave their homes months before they give birth and stay with relatives.
Their companions, usually husbands, had to undergo antigen testing, which costs a lot. “Without enough resources, they barely get by and survive.”
Ms. Umingli said her community would have been open to traditional medicines and vaccinations if these were taught to them properly.
“Some are reluctant at first but with proper explanation and understanding, they were convinced and got their vaccine,” she said.
Apart from being ill-informed, there is also no extensive data regarding indigenous people affected by the pandemic.
“Disaggregated data could have provided more groups the significant information to support the efforts in the provision of medical and relief services,” Ms. Tajon said.
“Vaccine hesitancy is not the main cause of the low vaccination rate, but the accessibility of public health services and health education for the people,” Filipino Nurses United Secretary-General Jocelyn S. Andamo said in a text message.
Fear of vaccines among IPs is understandable, Maristela P. Abenojar, president of Filipino Nurses United, said in a Viber message. “This is an issue that must be addressed by the government by strengthening the public health system.”
Other health experts said the state should boost vaccination efforts and create an inclusive, nationwide health campaign.
“Unless virus transmission is stopped, no one will be safe from getting infected, and from the emergence of new variants,” Teodoro B. Padilla executive director of the Pharmaceutical and Healthcare Association of the Philippines, said in an e-mail.
“While vaccination is not mandatory, all efforts must be exerted to include the IPs as priorities, and address their specific needs and cultural backgrounds to secure their free, prior and informed consent,” he added.
The coronavirus has sickened 3.69 million and killed more than 60,000 Filipinos. Globally, half-a-billion people have been infected, with more than 6 million deaths, according to the Worldometer website, citing various sources including data from the World Health Organization.
“These figures show the catastrophic impact of COVID-19 on the lives and health of the people. Members of the IP communities have not been spared,” Mr. Padilla said
IPs should have access to correct information about the advantage of being vaccinated against COVID-19, Ms. Abenojar said.
Mr. Tena, the Dumagat tribesman, said the coronavirus is just a speck in a sea of government shortcomings. “COVID is not the biggest issue we face that is threatening our livelihood and way of life.”



